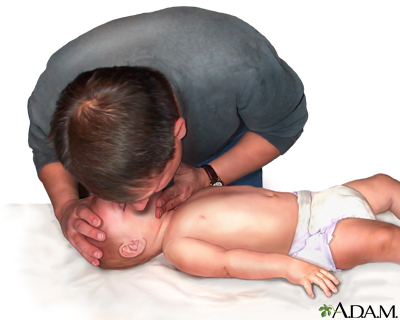
CPR - infant
Rescue breathing and chest compressions - infant; Resuscitation - cardiopulmonary - infant; Cardiopulmonary resuscitation - infant
CPR stands for cardiopulmonary resuscitation. It is a lifesaving procedure that is done when a baby's breathing or heartbeat has stopped. This may happen after drowning, suffocation, choking, or other injuries. CPR involves:
- Rescue breathing, which provides oxygen to the lungs.
- Chest compressions, which keep the blood flowing.
Permanent brain damage or death can occur within minutes if a baby's blood flow stops. Therefore, you must continue these procedures until the infant's heartbeat and breathing return, or trained medical help arrives.
Considerations
CPR is best done by someone trained in an accredited CPR course. The newest techniques emphasize compression over rescue breathing and airway, reversing long-standing practice.
All parents and those who take care of children should learn infant and child CPR. See www.americanheart.org for classes near you. The procedures described here are NOT a substitute for CPR training.
Time is very important when dealing with an unconscious baby who is not breathing. Permanent brain damage begins after only 4 minutes without oxygen, and death can occur as soon as 4 to 6 minutes later.
Machines called automated external defibrillators (AEDs) can be found in many public places, and are available for home use. These machines have pads or paddles to place on the chest during a life-threatening emergency. They automatically check the heart rhythm and give a sudden shock if, and only if, that shock is needed to get the heart back into the right rhythm. Make sure the AED can be used on infants. When using an AED, follow the instructions exactly.
Causes
There are many things that cause an infant's heartbeat and breathing to stop. Some reasons you may need to do CPR on an infant include:
- Choking
- Drowning
- Electrical shock
- Excessive bleeding
- Head trauma or serious injury
- Lung disease
- Poisoning
- Suffocation
Symptoms
CPR should be done if the infant has the following symptoms:
-
No breathing
No breathing
Breathing that stops from any cause is called apnea. Slowed breathing is called bradypnea. Labored or difficult breathing is known as dyspnea....
Read Article Now Book Mark Article - No pulse
-
Unconsciousness
Unconsciousness
Unconsciousness is when a person is unable to respond to people and activities. Doctors often call this a coma or being in a comatose state. Other c...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
First Aid
1. Check for alertness . Shake or tap the infant gently. See if the infant moves or makes a noise. Shout, "Are you OK"?
2. If there is no response, shout for help . Tell someone to call 911 and get an AED, if available. Do not leave the infant yourself to call 911 until you have done CPR for about 2 minutes.
3. Carefully place the infant on their back . If there is a chance the infant has a spinal injury, two people should move the infant to prevent the head and neck from twisting.
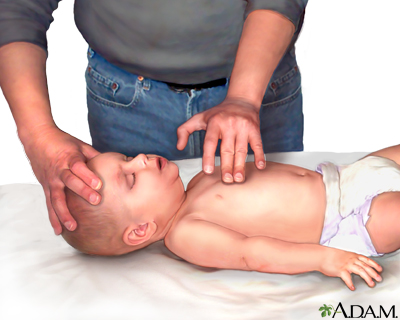
4. Perform chest compressions :
- Place 2 fingers on the breastbone -- just below the nipples. Make sure not to press at the very end of the breastbone.
- Keep your other hand on the infant's forehead, keeping the head tilted back.
- Press down on the infant's chest so that it compresses about one third to one half the depth of the chest.
- Give 30 chest compressions. Each time, let the chest rise completely. These compressions should be FAST and hard with no pausing. Count the 30 compressions quickly: ("1,2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30, off.")
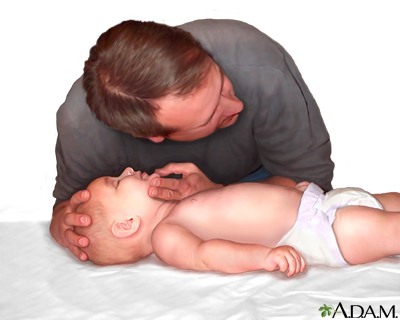
5. Open the airway . Lift up the chin with one hand. At the same time, tilt the head by pushing down on the forehead with the other hand.
6. Look, listen, and feel for breathing . Place your ear close to the infant's mouth and nose. Watch for chest movement. Feel for breath on your cheek.
7. If the infant is not breathing :
- Cover the infant's mouth and nose tightly with your mouth.
- Or, cover just the nose. Hold the mouth shut.
- Keep the chin lifted and head tilted.
- Give 2 rescue breaths. Each breath should take about a second and make the chest rise.
8. After about 2 minutes of CPR, if the infant still does not have normal breathing, coughing, or any movement, leave the infant if you are alone and call 911 . If an AED for children is available, use it now.
9. Repeat rescue breathing and chest compressions until the infant recovers or help arrives.
Keep rechecking for breathing until help arrives.
Do Not
-
Do NOT lift the infant's chin while tilting the head back to move the tongue away from the windpipe. If you think the baby has a
spinal injury
, pull the jaw forward without moving the head or neck. Do NOT let the mouth close.
Spinal injury
The spinal cord contains the nerves that carry messages between your brain and body. The cord passes through your neck and back. A spinal cord inju...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - If the infant has normal breathing, coughing, or movement, do NOT begin chest compressions. Doing so may cause the heart to stop beating.
When to Contact a Medical Professional
- If you have help , tell one person to call 911 while another person begins CPR.
- If you are alone , shout loudly for help and begin CPR. After doing CPR for about 2 minutes, if no help has arrived, call 911. You may carry the infant with you to the nearest phone (unless you suspect a spinal injury).
Prevention
Most children need CPR because of a preventable accident. The following tips may help prevent some accidents in children:
- Never underestimate what an infant can do. Assume the baby can move more than you think.
- Never leave an infant unattended on a bed, table, or other surface from which the infant could roll off.
- Always use safety straps on high chairs and strollers. Never leave an infant in a mesh playpen with one side down. Follow the guidelines for using infant car seats.
- Teach your baby the meaning of "don't touch". The earliest safety lesson is "No!"
- Choose age-appropriate toys. Do not give infants toys that are heavy or fragile. Inspect toys for small or loose parts, sharp edges, points, loose batteries, and other hazards.
- Create a safe environment. Watch children carefully, particularly around water and near furniture.
- Keep toxic chemicals and cleaning solutions safely stored in childproof cabinets.
-
To reduce the risk of
choking
accidents, make sure infants and small children cannot reach buttons, watch batteries, popcorn, coins, grapes, or nuts.
Choking
Choking is when someone is having a very hard time breathing because food, a toy, or other object is blocking the throat or windpipe (airway). A cho...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Sit with an infant while he or she eats. Do not allow an infant to crawl around while eating or drinking from a bottle.
- Never tie pacifiers, jewelry, chains, bracelets, or anything else around an infant's neck or wrists.
References
American Red Cross. Pediatric First Aid/CPR/AED Ready Reference . Revised 6/14. Dallas, TX: American Red Cross; 2014.
Berg MD, Schexnayder SM, Chameides L, et al. Part 13: pediatric basic life support: 2010 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation . 2010;122(18 Suppl 3):S862-S875. PMID: 20956229 www.ncbi.nlm.nih.gov/pubmed/20956229 .
Cukor J, Manno M. Pediatric respiratory emergencies. In: Marx J, Hockberger RS, Walls RM, et al, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice . 8th ed. Philadelphia, PA: Elsevier Saunders; 2014:chap 168.
Donoghue AJ, Berg RA, Nadkarni V. Pediatric resuscitation. In: Marx JA, Hockberger RS, Walls RM, et al, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice . 8th ed. Philadelphia, PA: Elsevier Saunders; 2014:chap 10.
Review Date: 4/12/2015
Reviewed By: Jacob L. Heller, MD, MHA, Emergency Medicine, Virginia Mason Medical Center, Seattle, WA. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.